It started with a conversation we weren't expecting. A neurologist mentioned — almost offhandedly — that the most frustrating part of their day wasn't the diagnostic complexity. It was the administrative overhead that came after the examination.
Scoring scales scattered across PDFs. Handwritten notes buried in paper charts. No way to track a patient's progression over time. They were spending more time organizing information than interpreting it.
 VOSS lives inside the clinical moment — not as another dashboard to check after the fact.
VOSS lives inside the clinical moment — not as another dashboard to check after the fact.
The Problem Nobody Was Solving
Neurological examinations are inherently structured. Tools like the NIH Stroke Scale and the Montreal Cognitive Assessment follow specific scoring protocols. Yet the way clinicians record these exams hasn't meaningfully changed in decades. It's still paper, or at best, a PDF you fill in and print.
"I can diagnose a complex movement disorder in 20 minutes. But documenting the exam and comparing it to last visit's scores? That takes longer than the exam itself."
We heard variations of this from multiple neurologists. The pattern was clear: the workflow was begging for a tool that was purpose-built, portable, and fast.
Why an iPhone App?
We debated this. A web app would have been easier to ship. An iPad would give us more screen real estate. But we kept coming back to one observation: neurologists carry their phones everywhere. Into exam rooms, on ward rounds, between clinics.
An iPhone app that could be used mid-examination to score a scale in real time, then immediately compared to historical data — that was the product.
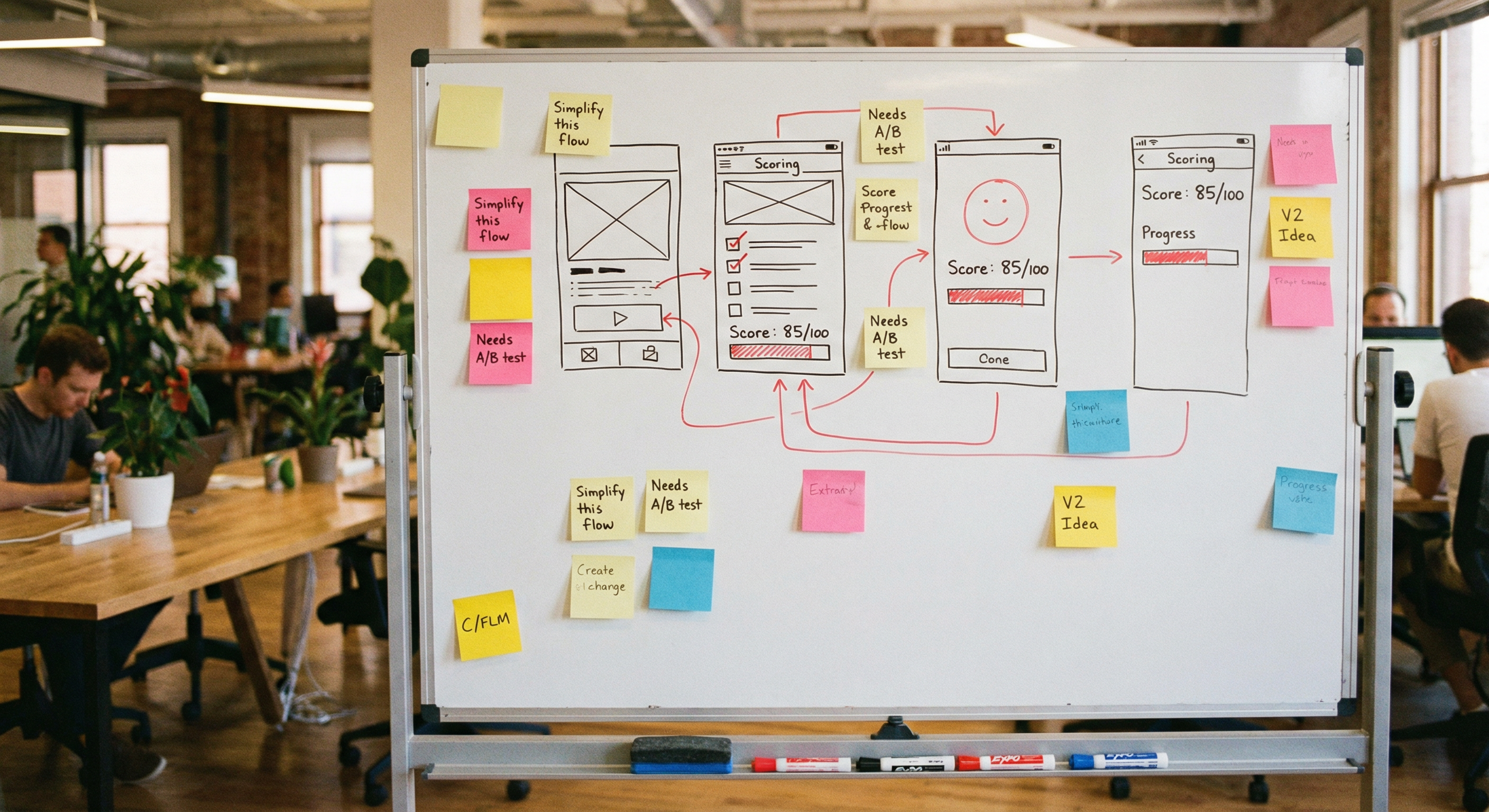 Early wireframes for VOSS. We gave ourselves four months to get a working prototype into a neurologist's hands.
Early wireframes for VOSS. We gave ourselves four months to get a working prototype into a neurologist's hands.
From Whiteboard to Prototype
We set a tight constraint: working prototype in under four months. That meant hard decisions early:
- Start with one scale. Get the workflow right first, build the architecture to support more later.
- On-device first. Patient data never leaves the device unless the clinician explicitly exports it. A trust decision, not just a privacy one.
- Design for speed. Every tap matters mid-patient encounter. We obsessed over reducing interactions.
The first prototype was rough — accurate but sterile. The second found the balance: rigorous enough to be clinically reliable, intuitive enough to need no tutorial.
What We Learned
Building for clinicians has near-zero tolerance for friction. If the app adds even 30 seconds to their workflow, it won't get used. And trust is everything — neurologists didn't ask how we built the app. They asked where the data was stored and who had access.
Those questions shaped our entire security architecture. The core insight hasn't changed: give clinicians a tool that fits their workflow, respects their time, and earns their trust. Everything else follows from that.
Interested in VOSS or Building Healthcare Tools?
We'd love to hear from clinicians, researchers, and anyone improving clinical workflows.
Get In Touch →